What Is Shock Wave Therapy and How Does It Work? A Comprehensive Technical Guide
Shock Wave Therapy (SWT), also known as Extracorporeal Shock Wave Therapy (ESWT), is a non-invasive, drug-free therapeutic modality that uses high-energy acoustic waves to treat a wide range of musculoskeletal disorders, chronic pain conditions, and tissue repair needs. Since its introduction in the 1980s—initially for breaking down kidney stones through extracorporeal shockwave lithotripsy (ESWL)—it has evolved into a cornerstone of physical therapy, orthopedics, sports medicine, and rehabilitation medicine, earning the reputation of a “bloodless scalpel” for its ability to deliver effective treatment without surgery or downtime.
This technical article explores the core definition, classification, working mechanisms (both physical and biological), technical parameters, and clinical applications of shock wave therapy, providing a detailed overview for medical professionals, therapists, and industry practitioners.
1. What Is Shock Wave Therapy?
In technical terms, a shock wave is a high-pressure, short-duration acoustic pulse that propagates through a medium (such as human tissue) at supersonic speeds, characterized by a rapid rise in pressure followed by a brief negative pressure phase. Unlike continuous ultrasound waves, which are periodic and low-amplitude, shock waves are discrete, high-amplitude pulses that deliver concentrated energy to targeted tissues—making them ideal for triggering biological responses that promote healing and pain relief.
Extracorporeal Shock Wave Therapy (ESWT) refers to the delivery of these shock waves from an external device to the body, without the need for invasive incisions. The therapy is classified into two primary types based on wave propagation and energy focus, each tailored to specific clinical needs:
1.1 Focused Shock Wave Therapy (FSWT)
FSWT generates high-energy shock waves that are concentrated into a small, precise focal point using reflectors or lenses within the device. These waves travel at speeds of up to 1500 meters per second, with peak pressure amplitudes significantly higher than other forms of shock wave therapy—up to 100 times greater than radial shock waves. Notably, FSWT’s energy intensifies with depth, allowing it to target deep tissues (up to 8–10 cm) such as bones, deep tendons, and ligaments, making it suitable for treating conditions like avascular necrosis of the femoral head, non-union fractures, and deep calcific tendinitis.
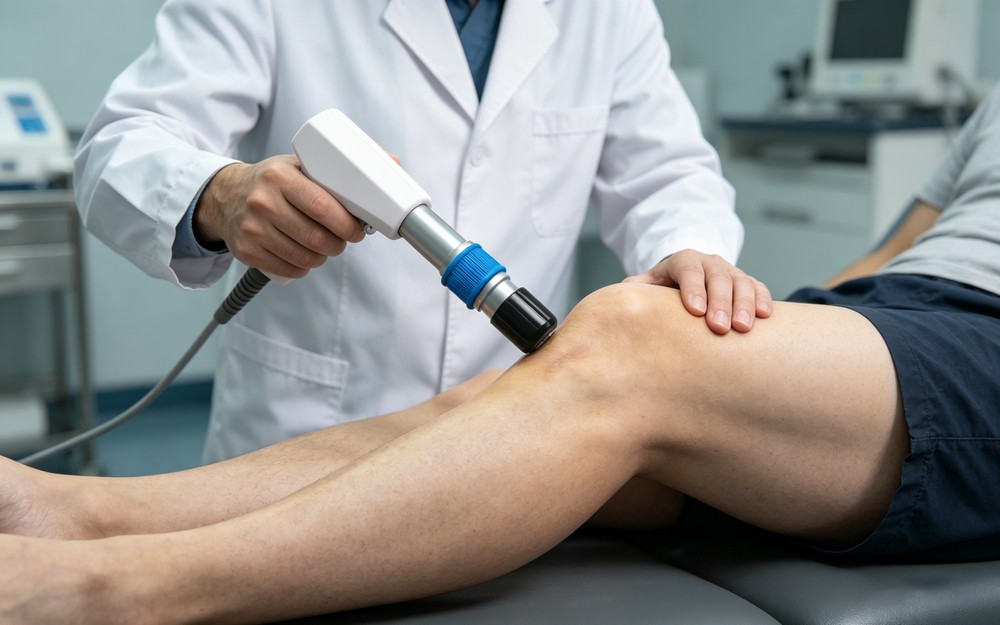
1.2 Radial Shock Wave Therapy (RSWT)
RSWT, also known as radial pressure wave therapy, produces spherical, diverging waves that propagate outward from the treatment head. Generated by a projectile accelerated by compressed gas striking the applicator, these waves have lower peak pressure (traveling at an average speed of 20 meters per second) and their energy dissipates rapidly with depth—losing 50% of energy per centimeter of tissue penetration, and nearly all energy by 2 cm depth. RSWT is primarily used for superficial soft tissue conditions, such as muscle strains, plantar fasciitis, and myofascial pain, due to its ability to cover a larger treatment area with gentle, diffused energy.
2. How Does Shock Wave Therapy Work? The Technical Mechanisms
The therapeutic effects of shock wave therapy stem from a combination of physical (mechanical) effects and biological responses triggered by the mechanical stimulus of the shock waves. This process, known as mechanotransduction, converts the mechanical energy of the shock waves into cellular and molecular signals that drive tissue repair, pain relief, and inflammation reduction.
2.1 Physical (Mechanical) Mechanisms
The physical effects of shock waves are the foundation of their therapeutic action, directly interacting with tissues to alter their structure and function:
- Cavitation Effect: As shock waves pass through tissue fluids, they create tiny bubbles (cavitation bubbles) that rapidly expand and collapse. This collapse generates micro-jets of fluid, which exert shear forces on surrounding tissues—loosening adhesions between tendons and fascia,疏通ing blocked microvessels, and improving local blood circulation. This effect is particularly effective for breaking down scar tissue and calcifications, such as those found in calcific tendinitis.
- Stress Effect: Shock waves create alternating positive and negative pressure cycles as they propagate through tissues. The positive pressure phase compresses tissues, while the negative phase stretches them, generating shear forces at the interface between different tissue types (e.g., bone and tendon). These forces can击碎 calcified deposits, stimulate bone remodeling, and trigger cellular responses that promote healing. For deep bone conditions like non-union fractures, this effect activates osteoprogenitor cells to accelerate bone regeneration.
- Energy Transmission: Shock waves are transmitted through the body using a coupling gel, which minimizes energy loss and ensures efficient delivery to the target tissue. The energy density (energy per unit area) of the shock waves—measured in mJ/mm²—is a critical parameter, as it determines the intensity of the therapeutic effect and is adjusted based on the condition being treated and the patient’s tolerance.
2.2 Biological Mechanisms
The physical effects of shock waves trigger a cascade of biological responses that drive long-term tissue repair and pain relief, extending beyond the immediate mechanical changes:
- Tissue Regeneration: Shock waves stimulate the proliferation and differentiation of fibroblasts (cells that produce collagen) and osteoblasts (bone-forming cells), promoting the synthesis of collagen and bone matrix. They also induce angiogenesis—the formation of new blood vessels—by upregulating growth factors such as VEGF (Vascular Endothelial Growth Factor), improving blood supply and oxygen delivery to damaged tissues. This accelerates the healing of tendons, ligaments, and bones, making it effective for chronic injuries and non-healing fractures.
- Analgesic (Pain-Relieving) Effect: Shock waves exert multiple pain-relieving effects: they block pain signals from reaching the central nervous system by inhibiting the activity of pain receptors (nociceptors); deplete local pain mediators such as substance P; and stimulate the release of endorphins (the body’s natural painkillers). This dual mechanism provides both immediate and long-term pain relief for chronic conditions like plantar fasciitis and tennis elbow.
- Anti-Inflammatory Effect: Shock waves reduce chronic inflammation by inhibiting the release of pro-inflammatory cytokines (e.g., TNF-α, IL-6) and activating anti-inflammatory cells such as macrophages. This helps resolve edema, reduce swelling, and alleviate pain associated with inflammatory conditions like tendinitis and osteoarthritis.
3. Core Technical Parameters of Shock Wave Therapy Devices
The effectiveness of shock wave therapy depends on precise control of technical parameters, which are adjusted based on the treatment target, tissue depth, and patient condition. Key parameters include:
- Energy Density: Ranges from 0.08 to 0.6 mJ/mm² for RSWT (superficial tissues) and 0.1 to 6.0 bar (or higher) for FSWT (deep tissues). Higher energy densities are used for calcified or deep lesions, while lower densities are suitable for sensitive areas or superficial soft tissues.
- Frequency: Typically 1–22 Hz, with lower frequencies (1–5 Hz) used for deep tissues and higher frequencies (10–22 Hz) for superficial tissues. Frequency determines the number of shock waves delivered per second, influencing the total energy delivered during a session.
- Penetration Depth: Ranges from 0.5–2 cm for RSWT (superficial) and up to 8–10 cm for FSWT (deep). This parameter is determined by the type of shock wave (focused vs. radial) and the applicator design.
- Wave Generation Technology: Devices generate shock waves using four primary technologies: electrohydraulic (high energy, focused, used for deep bone conditions), electromagnetic (stable, versatile, ideal for rehabilitation), piezoelectric (high precision, used for small, targeted areas), and pneumatic (radial, cost-effective, used for superficial tissues). Each technology has unique advantages and clinical applications.
4. Clinical Applications and Indications
Shock wave therapy is widely used in medical and rehabilitation settings, with proven efficacy for a range of conditions. Its applications are categorized into three main areas:
4.1 Musculoskeletal and Pain Conditions
This is the most common application of shock wave therapy, covering both chronic and acute conditions:
- Soft tissue disorders: Plantar fasciitis, Achilles tendinitis, tennis elbow (lateral epicondylitis), golf elbow (medial epicondylitis), shoulder calcific tendinitis, myofascial pain, and muscle strains.
- Bone and joint disorders: Osteoarthritis (knee, hip, shoulder), non-union fractures, avascular necrosis of the femoral head, bone marrow edema, and tibial stress syndrome.
4.2 Sports Rehabilitation
In sports medicine, shock wave therapy is used to treat acute sports injuries (e.g., muscle sprains, tendon strains) and accelerate post-training recovery. It helps reduce muscle soreness, improve tissue flexibility, and speed up the healing of sports-related injuries, making it a valuable tool for athletes at all levels.
4.3 Other Emerging Applications
Beyond musculoskeletal conditions, shock wave therapy is being explored for aesthetic purposes (cellulite reduction, fat reduction, and stretch mark improvement) and wound healing (chronic diabetic ulcers, non-healing wounds) due to its ability to promote angiogenesis and tissue regeneration. It is also being studied for the treatment of neurologic disorders, such as reducing spasticity in stroke patients.
5. Key Advantages and Contraindications
5.1 Advantages
- Non-invasive: No surgery, incisions, or anesthesia required, reducing the risk of infection and downtime.
- Drug-free: Avoids the side effects of pain medications or anti-inflammatory drugs, making it suitable for patients with drug allergies or contraindications.
- High efficacy: Clinical studies show a success rate of 70–90% for most musculoskeletal conditions, with results visible after 3–5 sessions (each 5–15 minutes long).
- Versatile: Suitable for a wide range of conditions and tissue types, from superficial muscles to deep bones.
5.2 Contraindications
Shock wave therapy is not suitable for all patients. Contraindications include:
- Pregnancy (risk of harm to the fetus).
- Bleeding disorders or patients taking anticoagulants (risk of bleeding).
- Malignant tumors (may stimulate tumor growth).
- Infected or inflamed tissues (may worsen inflammation).
- Patients with pacemakers or other implanted medical devices (shock waves may interfere with device function).
- Children with unclosed epiphyses (risk of disrupting bone growth).
6. Conclusion
Shock Wave Therapy (ESWT) is a sophisticated, evidence-based therapeutic modality that leverages high-energy acoustic waves to trigger physical and biological responses for tissue repair, pain relief, and inflammation reduction. Its classification into focused and radial types allows for targeted treatment of both deep and superficial tissues, making it a versatile tool in orthopedics, physical therapy, sports medicine, and beyond.
By understanding its technical mechanisms—from cavitation and stress effects to cellular regeneration and analgesia—medical professionals can optimize treatment parameters for individual patients, ensuring safe and effective outcomes. As research continues, shock wave therapy is likely to expand into new applications, solidifying its role as a key non-invasive treatment option for musculoskeletal and other conditions.